2015 Pipeline Report: Burning Bright
The science of drug discovery is back on script-and the stars are cued up for a new generation of breakthrough therapies. But is pharma ready to raise its game and cut a deal with all those "prove it to me" payers?
Tracking new therapies as they wind their way through development, regulatory approval, and payer acceptance can be like waiting for paint to dry and then repainting in a different color. It's a slow process and far from linear.

(GETTY IMAGES / PIXELPARTICLE)
This is especially true for potentially groundbreaking drugs, disruptive technologies that completely upend markets and patient care. The lag time between that first flickering glimmer of hope and an accepted therapy can be measured in decades. And, all too often, agents that seem hopeful in the lab and early clinical trials fizzle on further investigation.

Josh Baxt
But then there are those rare moments when the stars align and truly astounding therapies make their way into the world, providing improved care and big returns. In the next few years, cancer immunotherapies seem likely to enter the pantheon of big winners. And they may not be alone. Besides the buzz around a cure for hepatitis C virus, there are exciting drugs for heart failure and cholesterolemia coming into play. On a smaller scale, companies are embracing new therapies for rare diseases. Stem cells are making real forays into late-stage trials.
This year's pipeline report will check in on these emerging technologies, as well as potential therapies to address metabolic and neurodegenerative diseases. There's a lot to like in the pipeline and more than a little competitive drama to make it really interesting.
Immuno-oncology: The elegant solution
For Trekkers, there's nothing better than watching a Klingon or Romulan ship lose its invisibility cloak and get blasted out of space. On the cellular level, similar action is driving the excitement around programmed death 1 (PD-1)/programmed death ligand 1 (PD-L1) checkpoint inhibitors: the opportunity to reveal cancer and unleash the immune system against it.
"There's genuine enthusiasm among oncology experts," says Seamus Fernandez, managing director of Major and Specialty Pharmaceuticals at Leerink Partners. "There's evidence of activity in more than five different tumors and signals of activity in as many as 14. We forecast a $36 billion immuno-oncology market by 2025."
That's a large pie and there's been a lot of jostling to get the biggest piece. Bristol-Myers Squibb's cytotoxic T lymphocyte antigen-4 (CTLA-4) inhibitor Yervoy (ipilimumab) was first out of the gate, but there are several other agents poised to hit the market.
In September, Merck's PD-1 blocker Keytruda (pembrolizumab) received accelerated approval from the FDA to treat melanoma and the company is researching the drug against non-small cell lung cancer (NSCLC) and other indications. In its World Preview 2014 Outlook report, EvaluatePharma forecasts Keytruda sales of $4.06 billion by 2020.
That's a great start, but it's unclear whether Merck's advantage will hold out over the long haul. The competition will be fierce in the PD-1/PD-L1 space. With the huge potential market, this could be the equivalent of the Oklahoma land rush for the usual pharma titans. However, Stephanie Hawthorne, senior director at Kantar Health, notes that, for now in melanoma, Merck is in the driver's seat compared to BMS's PD-1 inhibitor Opdivo (nivolumab), which is a few months (or possibly longer) behind Keytruda in the US.
"It's a big advantage for Merck being first-to-market," says Hawthorne. "Based on the available data, they both look really efficacious, and they're fairly well tolerated compared to Yervoy. BMS's saving grace might be the combination of Opdivo and Yervoy they are studying. The survival data we've seen for it so far is really impressive, and that could trump Merck's lead."
Hawthorne's point was underscored in late September when BMS released data at the European Society for Medical Oncology (ESMO) showing that Opdivo achieved a 32% response rate against advanced melanoma in patients who had previously been treated with Yervoy. The control group, which received traditional chemo, had an 11 % response.
While Keytruda was first in the US, Opdivo was approved for melanoma in Japan in July, under a deal with BMS partner Ono Pharmaceuticals. The ESMO data will only support BMS's showing in the US. The FDA has given Opdivo fast track designation in NSCLC, melanoma, and renal cell carcinoma (RCC) and breakthrough therapy designation for Hodgkin's lymphoma. In September, BMS announced that both the FDA and European Medicines Agency (EMA) have accepted Opdivo for accelerated review for melanoma. The FDA PDUFA date is March 30, 2015.
"Opdivo is the most valuable pipeline drug in development at the moment," says Lisa Urquhart, editor of Evaluate's editorial team, EP Vantage. "The data from studies is showing some impressive advances in both overall survival and disease progression."
EvaluatePharma pegs Opdivo's potential sales at $6 billion by 2020. The company believes Opdivo could be approved for melanoma in the US next year. Meanwhile, Hawthorne expects approval for the Opdivo/Yervoy combination in early 2016.
That's in melanoma. Opdivo may even have a more clear-cut advantage in being first-to-market for NSCLC, where BMS has already submitted its drug for approval while Merck is still completing Phase III trials.
A crowded field
The PD-1/PD-L1 approach is generating a lot of enthusiasm for good reason. Early results have shown great efficacy in many indications, including underserved areas, such as bladder and head and neck cancers. The possibility of producing an agent that can target multiple cancers is raising heart rates throughout the pharma industry.

"These drugs are all across the board," says Hawthorne. "I'm not sure there's a tumor type that's not being touched: renal cell cancer, head and neck, bladder, and Hodgkin's lymphoma. It's just an indication of how huge and impactful these could be for patients."
Again, this is underscored by Merck results, also released at ESMO, which showed a 24% response rate for Keytruda against bladder cancer.
Genentech/Roche's PD-L1 offering, MPDL3280A (RG-7446), is in trials for NSCLC, melanoma, RCC, and bladder cancer. The company received breakthrough designation for this last indication. EvaluatePharma puts sales at $2.93 billion by 2020, while the Thomson Reuters Cortellis database puts them at $1.2 billion by 2019.
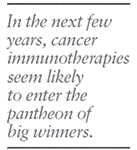
MedImmune/AstraZeneca is also in the race with PD-L1 drug MEDI-4736, primarily targeting NSCLC. Also shared at ESMO, a small 18-person study showed a 28% response to MEDI-4736 combined with the CTLA-4-directed antibody tremelimumab. Cortellis projects MEDI-4736 sales at close to $1.1 billion by 2019.
"We're just at the tip of the iceberg for immuno-oncology, but the enthusiasm is certainly warranted because of the kinds of responses and the tumors being opened up," says Fernandez. "The field is about as exciting and confusing as you could possibly imagine."
The combo conundrum
With these fantastic response rates in aggressive cancers, how will PD-1/PD-L1 inhibitors redefine patient care? As monotherapies? In combination with other types of immuno-oncology drugs? Or will they be combined with the new generation of targeted chemotherapies?

"The best-case scenario, these agents are working in 35 to 50% of melanoma patients as single agents," says Fernandez. "Worst-case scenario, maybe they're working in 15 or 20%. There's a strong conviction that multiple mechanisms are going to be relevant in various different tumors."
How this will play out is subject to much debate. If Fernandez's more optimistic scenario proves accurate, these checkpoint agents could be extremely successful monotherapies, which could have a profound impact on standards of care.
"This could be very disruptive," says Hawthorne. "Whereas you're used to treating lung cancer with cisplatin or carbo-taxol first line, you might get Opdivo and that could push those drugs out."
Hawthorne anticipates that both clinical and commercial factors will drive companies to test their more traditional therapies in combination with the emerging checkpoint inhibitors.
"If the drug has the potential to displace you, then it makes sense to go in combination with it," says Hawthorne.
In addition, there's the long-term possibility of pairing a PD-1/PD-L1 with emerging immunotherapies that target different mechanisms. Just over the horizon, chimeric antigen receptor (CAR-T) therapies could make a big impact. Unlike PD-1/PD-L1 inhibitors, which unchain immunity, CAR-Ts activate the immune system, which offers intriguing possibilities, as well as possible dangers.
"My wariness would be around the potential side effects," says Hawthorne. "If you're simultaneously upregulating the immune system and taking the brakes off, that could go kind of crazy."
At this point, Novartis is first in the CAR-T line with CTL019, which received breakthrough designation from the FDA in July for acute lymphoblastic leukemia (ALL). The drug is currently in Phase II trials.
However, CAR-T therapy may not have an easy path. A Juno Therapeutics/Memorial Sloan-Kettering study for aggressive non-Hodgkin's lymphoma (NHL) was halted recently after two patients died from cytokine release syndrome, one of the apparent risks of taking the brakes off the immune system. While the study was only delayed, this event underscores potential concerns about CAR-T therapies.
Another interesting immuno-oncology therapy is Amgen's blinatumomab, a bi-specific T-cell engager (BiTE). Blinatumomab received breakthrough therapy designation for ALL in July, and Amgen has filed for early approval. At Leerink Partners' Healthcare Insights Conference in July, a number of experts expressed their belief that this drug is an interesting proof-of-concept; however, they were also concerned about neurotoxicity. Thomson Reuters puts potential sales at $325 million by 2019.
There are too many immunotherapies to list here, which is great news for cancer patients. Ultimately, PD-1/PD-L1 may form the backbone for a variety of combinations. This is based on efficacy, as well as a complementary mechanism of action, but there's also a practical measure. With so many different combinations, it would be virtually impossible to test them all.
There are also cell-based therapies that look promising. For example, Aduro BioTech recently received breakthrough designation for its combination immunotherapy CRS-207 and GVAX. CRS-207 uses engineered Listeria to stimulate an immune response against mesothelin. GVAX is made from pancreatic cancer cells modified to secrete GM-CSF, which also provokes an immune response.
"They did a very small phase I study: seven patients were treated and some lived for two or three years," says Ravi Kiron of BioPharma Strategy Advisors. Phase II results from early 2014 were also quite promising. They showed the combination therapy doubled one-year survival for patients with metastatic pancreatic ductal adenocarcinoma. The combo is currently in a phase IIb trial. "These cell-based therapies have a lot of potential," adds Kiron.
"The stakes get a lot more interesting and a lot more confusing," says Fernandez. "We are going to see a significant number of mixed successes and disappointments as we move forward with these different combinations."
Targeted oncology agents
While immunotherapies may hold the greatest upside, there are still a variety of more traditional treatments in the oncology pipeline.
First on the list are the poly ADP ribose polymerase (PARP) inhibitors, which encourage cancer cell death by limiting this DNA-repair enzyme. They include veliparib from AbbVie; rucaparib from Clovis Oncology/Pfizer; Lynparza (olaparib) from AstraZeneca; and BMN-673 from BioMarin. Their oral administration makes them particularly exciting.
Veliparib is being developed for triple-negative breast cancer and NSCLC. The drug showed a 52% response rate against breast cancer in a study that combined it with carboplatin and paclitaxel. AbbVie recently announced a pivotal Phase III study for patients with advanced breast cancer. The company is also conducting a Phase II trial for NSCLC. Thomson Reuters projects sales at $350 million by 2019.
Meanwhile, in a Phase II study, rucaparib showed a 93% disease control rate in BRCA-positive ovarian cancer. Thomson has rucaparib at $414 million by 2019.
Clovis has also earned breakthrough designation for its epidermal growth factor receptor (EGFR) blocker CO-1686 for lung cancer. At the 2014 ASCO Annual Meeting, Clovis unveiled excellent progression-free survival in a combo Phase I/II study.
The company will have major competition from AstraZeneca's AZD9291, which targets both EGFR and the resistance mutation T790. AstraZeneca is partnering with Roche, and the drug is currently in pivotal trials. They plan to file with regulators in the latter part of 2015, which seems like a long way off. Thomson Reuters estimates $761 million in sales in 2019.

Then there are the cell cycle regulating cyclin-dependent kinase 4 (CDK4) and CDK6 inhibitors, which show great potential for adjuvant treatment. At the front of the pack is Onyx/Pfizer's palbociclib. Pfizer has recently submitted a new drug application (NDA), in combination with letrozole, to treat advanced ER-positive, HER2-negative breast cancer. Data submitted at the AACR Annual Meeting showed a progression-free survival of 20.2 months. EvaluatePharma predicts palbociclib will have worldwide sales in the $2.95 billion range by 2020. Thomson Reuters Cortellis puts sales at $2.02 billion in 2019.
Another CDK4/CDK6 candidate is Eli Lilly's abemaciclib for metastatic breast cancer and NSCLC. Cortellis forecasts $306.2 million for that drug.
A revolution in heart failure
Heart failure is an underserved health area that is continuing to grow. Decision Resources Group recently estimated it will expand from $2.9 billion in 2013 to $8.9 billion in 2023. Breakthroughs have been limited for some years, so the field is wide open for promising therapeutics.
"Heart failure is very common and getting more common, very expensive in terms of co-morbidities and really underserved," says Les Funtleyder, a healthcare portfolio manager at E Squared Asset Management and member of Pharm Exec's Editorial Advisory Board.
Few drugs are generating more enthusiasm than Novartis' heart failure and hypertension treatment LCZ696. The drug has novel mechanisms, combining sacubitril to preserve peptides that lower blood pressure and valsartan to improve vasodilation. There haven't been any major improvements in heart failure therapies in decades. EvaluatePharma puts sales at $1.3 billion by 2020, while Thomson Reuters has them at $1.8 billion in 2019. Both estimates may be conservative.
Data from a pivotal Phase III trial showed the drug reduced the risk of death by 20%, compared to an angiotensin-converting-enzyme (ACE) inhibitor, as well as dramatically reducing the risk of hospitalization. There's a lot of excitement that this new drug could supplant ACE inhibitors and ARBs.
"We're forecasting $6 billion of peak sales, but that number could be low by a factor of 50% or even a 100%," says Seamus Fernandez. "LCZ696 could be a Plavix-like product."
This enthusiasm appears to be widespread.
"LCZ696 has been described as a game changer and there are some that believe that because of its mortality benefit it should become the standard of care replacing ACE inhibitors and ARBs, especially given its very clean safety profile," says Urquhart. "The market was also quick to wake up to its potential and after the Paradigm-HF trial was stopped early in March because of its conclusive benefits."
By contrast, Novartis' other heart failure drug has hit hard times. In May this year, the FDA rejected Novartis' biologics license application (BLA) for Serelaxin. A synthetic human relaxin 2 hormone, Serelaxin has breakthrough designation but the FDA needed more efficacy data for approval and had issues with the trial design. Novartis has been conducting a large Phase III trial and hopes the results, expected in 2016, will sway the FDA.

Serelaxin is a tantalizing prospect for both Novartis and analysts. In addition to the potential one-two punch with LCZ696, acute heart failure is a serious unmet need, with clinicians looking for successors to beta blockers, developed in the 1960s, and ACE inhibitors, developed in the '80s.
"There hasn't been a product to advance the in-hospital treatment for heart failure in somewhere between 30 and 50 years," notes Fernandez.
Fernandez styles Serelaxin a dark horse. However, if Novartis can get past the regulatory hurdles, Leerink Partners projects Serelaxin could be worth two to three billion dollars. By contrast, EvaluatePharma puts its sales at $484 million by 2018.
Raising HDL, Lowering LDL
There's a lot of work being done on LDL cholesterol, and a lot of skepticism to match. There could be an upcoming battle between proprotein convertase subtilisin kexin 9 (PCSK9) inhibitors and cholesterylester transfer protein (CETP) inhibitors, or not. Both approaches have great potential and flaws. The PCSK9 inhibitors seem to have a cleaner path towards approval. However, administration and compliance could be an issue.
"You're introducing an injectable and an antibody to treat an asymptomatic condition," says Fernandez. "People tend to be less compliant."
Leerink Partners believes there's a potential $10 billion worldwide market by 2030 for the four leading PCSK9 inhibitors from Amgen and Sanofi/Regeneron—the obvious leaders—followed by Pfizer and Lilly. The investment bank projects $4 billion by 2020.
Sanofi/Regeneron's alirocumab and Amgen's evolocumab seem pretty evenly matched, and the market may respond in kind. EvaluatePharma puts sales by 2018 at around $1 billion and $777 million, respectively.
Pfizer's bococizumab showed great results in a Phase IIb trial, significantly reducing LDL in patients also treated with statins. EvaluatePharma puts their sales at $231 million by 2018.
CETP inhibitors are administered orally but must contend with the long shadows of Pfizer's torcetrapin, which, unfortunately, had deadly side effects, and Roche's dalcetrapib, which simply wasn't effective. However, Merck's anacetrapib and Lilly's evacetrapib seem to be better at raising HDL and lowering LDL and are worth watching. Thomson Reuters has anacetrapib sales at $759 million by 2019 and evacetrapib at $373 million in the same time period.
"There's more consistency on the PCSK9 side," says Fernandez. "We don't have the same evidence with CETP inhibitors. However, if they work, and they may simply work by lowering LDL, they are oral products and might be the larger class."
Diabetes and obesity
In the immediate future, it seems like the diabetes market will be more evolutionary than revolutionary, governed by refinements in insulin delivery rather than major breakthroughs. Still, there are improvements to be made and healthy profits on top of that.
Case in point, Sanofi's Toujeo (insulin glargine), a reformulated long-lasting insulin, could preserve the company's income stream as Lantus loses patent protection. The FDA accepted Toujeo's NDA in July, and approval is expected in the first half of 2015. EvaluatePharma's projection comes in at $1.4 billion in sales by 2018. Thomson Reuters forecasts $1.6 billion by 2019.
Lilly/Boehringer's insulin glargine, Basaglar, was given tentative approval by the FDA in August, but Sanofi is claiming patent infringement. As a result, approval has been delayed for up to 30 months while the case makes its way through the courts. EvaluatePharma projects $401 million in sales by 2018.
Lilly/Boehringer are also working on insulin peglispro, an insulin analog for type 1 and type 2 diabetes. A recently concluded trial showed daily treatment compared favorably to insulin glargine. Lilly plans to submit insulin peglispro in early 2015. EvaluatePharma estimates sales of $406 million by 2018.
Focusing on type 2 diabetes, Lilly's long-acting glucagon-like peptide-1 (GLP-1) agonist Trulicity (dulaglutide) received FDA approval in September. GLP-1 is a hormone that balances blood sugar, making it a particularly tempting target for type 2 diabetes treatments. With EvaluatePharma projecting sales of $912 million by 2018, Trulicity could be bad news for Novo Nordisk and AstraZeneca.
"We think Trulicity could be a $1.5 billion drug and a meaningful competitor to Novo's Victroza," notes Fernandez. "I think it's going to do a lot of damage to AstraZeneca's Bydureon."
However, Novo has big plans for Victoza (liraglutide), which has recently been found safe and effective against obesity. In September, an FDA panel voted to recommend the drug for approval for that indication.
Perhaps more interesting, Novo has combined liraglutide with long-lasting insulin degludec (Tresiba) to create IDegLira for type 2 diabetes. Recent data have shown the drug works better than liraglutide and insulin degludec alone. Thomson Reuters puts IDegLira at $815 million by 2019. EvaluatePharma estimates $517 million by 2018.
Merck's omarigliptin, a dipeptidyl peptidase-4 (DPP-4) inhibitor to treat type 2 diabetes, is continuing through fairly massive Phase III trials. Taken weekly, the drug may reduce glucose as well as daily treatments. EvaluatePharma pegs sales at $412 million by 2018.
Zafgen's obesity drug Beloranib, which modulates fatty acid metabolism, is turning heads. A Phase II trial in 2013 produced rapid weight loss in severely obese patients and was well-tolerated. An effective weight loss drug with few side effects could have tremendous potential. This is definitely one to watch.
Neurodegenerative diseases
It would be wonderful to highlight a number of promising agents that could improve cognitive function in Alzheimer's disease patients. Billions have been spent on such treatments, most of them targeting amyloid plaque, and none of them have come through.
"There are so many bodies on the side of the road, it's almost as if the safe thing is to bet against any drug trying to affect cognitive function in Alzheimer's disease," says Ritu Baral, senior analyst, Biotechnology Equity Research managing director at Cowen and Co.
While there's no joy on the disease-modifying side, there are other efforts to mitigate some of the symptoms associated with Alzheimer's and other neurodegenerative conditions. Avanir's AVP-923, which combines ordinary dextromethorphan with the heart rhythm treatment quinidine, may have promise to treat the agitation associated with Alzheimer's. Avanir released positive Phase II results in September and is meeting with the FDA and EMA to discuss next steps.

"Agitation is the No. 1 driver behind hospitalization and institutionalization for Alzheimer's disease," notes Baral. "Agitation and aggression make it impossible to care for patients in the home setting."
Otsuka and Lundbeck are working on brexpiprazole for schizophrenia and major depressive disorder (MDD), as well as Alzheimer's-related agitation. The FDA has accepted the NDA for schizophrenia and as an adjunct treatment for MDD; the PDUFA date is set for July 2015. Thomson Reuters predicts potential sales of $1.43 billion by 2019. EvaluatePharma pegs sales at $763 million by 2018.
The pipeline is more promising in multiple sclerosis, as these drugs can target the underlying immune response. For example, Genentech/Roche's CD20 inhibitor ocrelizumab for relapsing-remitting MS is currently in Phase III trials and has been shown to reduce inflammatory brain lesions. Ocrelizumab is projected by EvaluatePharma to sell around $355 million by 2018. Thomson Reuters is a bit more bullish at $578 million by 2019.
Meanwhile AbbVie and Biogen Idec are working on the IL-2 receptor inhibitor Zinbryta (daclizumab), which treats relapsing-remitting MS. Recent data showed patients on the drug experienced a significant reduction in relapse when compared to Avonex, which had $3 billion in sales in 2013. EvaluatePharma projects $320 million by 2018 for Zinbryta, while Thomson Reuters goes higher at $829 million by 2019.
Bioden Idec's Plegridy was recently approved in the US as a weekly replacement for the daily Avonex. However, analysts are not universally enthusiastic about its prospects.
"The drug is approved in Europe and was supposed to be the natural, longer-acting successor to Avonex, which came off patent last year," says Lisa Urquhart at EvaluatePharma. "However, the lure of fortnightly dosing over weekly Avonex does not appear to be floating too many boats, and consensus sales forecasts for the drug have fallen significantly recently. At the moment, they are $537 million in 2018, nowhere near the $3 billion Avonex pulled in last year."
Also, there may be a little hope for patients with Huntington's disease. Early in the year, Raptor announced positive 18-month results on a three-year Phase II/III trial for RP103. In the study, total motor score progression was 32% slower in the RP103 group. An extended and delayed-release formulation of cysteamine bitartrate, RP103 recently received orphan drug designation from the European Commission. While it's still early in the process, good news is scant in Huntington's, so something to watch.

Rare diseases
Orphan disease therapies are becoming more and more popular with both big pharma and biotechs. The combination of exclusivity and a more streamlined path to market have made them increasingly appealing.
But while the orphan drug market has seen astronomical growth, there's been increasing push-back from payers over the prices for these medications. Given that cost containment is a central tenet of healthcare reform, it's unclear how six-figure prices will fare in the long run. To complicate the picture, patient advocacy groups have become increasingly engaged and will fight any measures that limit access. Given this environment, will payers balk at the growing slice of the pie going to specialty medications? No answers yet, but the implications are big.
At the top of the growing list of orphan drugs, Vertex may have a genuine blockbuster with its combination of lumacaftor and Kalydeco (ivacaftor) for cystic fibrosis. (CF) Recent Phase III results have been positive, though not overwhelming, showing the combo does improve lung function, just not as much as everyone would like.
Still, the drug has received FDA's breakthrough therapy designation and approval would dramatically increase the number of CF patients who could be treated with Vertex therapies. Right now, Kalydeco only helps around 4%, while the combination would cover around 50% of CF patients. Thomson Reuters puts the potential sales at $3.7 billion by 2019. Vertex is expected to file in the US and Europe by the end of the year.
Alexion acquired Enobia in 2012 and with it came asfotase alfa (ALXN-1215), which treats hypophosphatasia, an often deadly form of rickets. Alexion scooped up breakthrough therapy designation in 2013 for the enzyme replacement drug. A recently concluded study showed that five-year survival on the drug was 89%, compared to 27% for patients who received no treatment. The company submitted a rolling BLA in April. Thomson Reuters puts potential sales at $578 million by 2019.
There are a number of agents in the pipeline to treat Duchenne muscular dystrophy (DMD), which currently has few therapeutic options. One of these is Translarna (ataluren) from PTC. The small-molecule drug treats nonsense mutations in the dystrophin protein and was recently given conditional approval by the European Commission.
Prosensa's RNA drug drisapersen, an exon-skipping therapy, appears to be back from the dead. A Phase III study showed little advantage over placebo; however, additional data convinced the FDA to take another look. Drisapersen has breakthrough therapy status and the company is moving forward with an NDA.
Sarepta, which also takes an exon-skipping approach, is seeking early approval for its RNA drug eteplirsen, also for DMD. The company has experienced a bad combination of up and down trial results and corporate boardroom drama, but appears to be poised to submit the NDA for its DMD therapy. When approved, drisapersen and eteplirsen should be direct competitors.
Fabry disease is caused by mutations in the alpha-galactosidase A enzyme, which leads to fat build-up and a variety of painful and debilitating symptoms. There are a couple of approved Fabry treatments (Fabrazyme and Replagal), but they require weekly infusions that are especially difficult for children. However, Amicus has developed migalastat, a small-molecule drug that could help patients with less severe disease.
"One of the things people forget about enzyme-replacement therapies is that they require a significant amount of chair time," says Ritu Baral. "This has the potential to be a game changer in Fabry treatment because of its oral delivery."
Migalastat is designed to treat people who have some enzyme activity, as many as 50% of Fabry patients. The drug has had an up and down path and GlaxoSmithKline pulled out of their deal with Amicus, but improved Phase III results have put the drug back on track. Thomson Reuters estimates sales at $99 million.
BioMarin has a promising therapy for Pompe disease, a lysosomal storage disorder that causes weakness and respiratory issues. BMN-701 has received FDA orphan drug designation and is in Phase III trials. Thomson Reuters puts potential sales at $163 million by 2019.
Stem cells
Stem cells have been long on potential but short on immediate benefit. However, that may be gradually changing, as a number of therapies are making their way through Phase III trials. Though it's difficult to gauge what kind of impact these therapeutics will have on health or markets, this might be the tip of the iceberg, and we will finally see some actual stem cell therapies make their way to patients.
While the majority of press has been devoted to the hand-wringing around embryonic stem cells and the blinding coolness of induced pluripotent stem cells, the therapies closest to market often rely on more differentiated cells. These treatments are a bit sparse on data and projections but they're interesting to watch and are likely a harbinger for bigger things to come.
One good example is Revascor (CEP-41750), Teva/Mesoblast's adult mesenchymal stem cell treatment for heart failure, which is currently in a large, 1,730-patient pivotal Phase III trial. Outcomes won't be available for some time but previous results have been encouraging, though they have come from small samples. While it won't be the blockbuster Novartis' LCZ-696 is expected to be, it could make a significant impact.
Gamida Cell is moving forward with its Phase III trial for StemEx, a therapy for blood cancers, such as leukemia and lymphoma. The therapy has orphan drug designation and fast track status and is intended for patients who cannot find a marrow donor. Gamida has been changing partners lately, with Teva dropping out and Novartis being an on-off-on suitor.
In earlier stages, both Stem Cells Inc. and Asterias are working on treatments for chronic spinal cord injuries, Asterias is picking up where Geron left off. In addition, there are a number of early-phase studies investigating the possibility of inhibiting cancer stem cells, which may provide a well of slow-growing cells that continuously reinvigorate certain tumors. Celgene has invested heavily in therapies that address cancer stem cells.
Odds and ends
As the year ends, Ebola is dominating the news and there's palpable hope that new treatments will rescue the world from a full-blown pandemic. Mapp, Sarepta, and Tekmira are collaborating with the World Health Organization, Wellcome Trust, and other organizations to begin trials in West Africa. In addition, OncoSynergy has received orphan drug designation for OS2966, which targets CD29 to treat glioblastoma and other aggressive cancers. But CD29 also plays a role in Ebola and the company is planning a trial.
Further out on the science frontier, Spark Therapeutic is in a Phase III for its ophthalmological gene therapy agent, which uses a viral vector to deliver the RPE65 gene to treat a number of eye conditions. This is a good candidate to be the first gene treatment approved in the US, but it certainly won't be the last. Gene therapy has risen quickly from being moribund to red hot.
Another area that's gaining ground is antibiotics. The Generating Antibiotic Incentives Now (GAIN) provisions are driving innovation in anti-bacterials in the same way the Orphan Drugs Act supported work on rare diseases. One interesting example is Cempra's solithromycin, which is in trials for community-acquired pneumonia and other infections. Thomson Reuters projects sales of $200 million by 2019.
Biosimilars are knocking on the door, but many questions remain about how they'll fare in the US market. Sandoz has filed a BLA for its version of Neupogen. Celltrion is right behind them with a biosimilar of Remicade. However, regulatory approval may be the easy part. Biosimilars still face patent battles, prospective price discounts remain hostage to the uncertainty around trial development costs, and there's no guarantee physicians will switch patients to these newer versions of established drugs.
And finally, far off on that distant horizon, there is keen interest in microbiota, the human body's friendly bacteria. Pfizer is partnering on drug candidates with Second Genome, a leader in this area, and there are a host of startup ventures coming out of the woodwork. This could be an interesting area for approval candidates in 2020.
Payer politics
As Gilead well knows from its Sovaldi experience, developing a groundbreaking therapy, and gaining FDA approval, doesn't guarantee blockbuster nirvana. Gilead has been a popular punching bag for Sovaldi's perceived high price, but it is hardly unique. A number of emerging therapies are generating sticker shock, particularly in oncology.
How will payers push back? There's a lot of discussion—at conferences, in the media, in Congress—but no clear consensus has emerged. Some payers are already asking for evidence of value and there are potential trends towards referencing across borders and closed formularies. This will be a complicated societal issue, as drug companies, payers, and consumers wrestle with the question: How much is too much?
Josh Baxt is a freelance science and healthcare writer. He can be reached at joshb@baxtcomm.com.
Addressing Disparities in Psoriasis Trials: Takeda's Strategies for Inclusivity in Clinical Research
April 14th 2025LaShell Robinson, Head of Global Feasibility and Trial Equity at Takeda, speaks about the company's strategies to engage patients in underrepresented populations in its phase III psoriasis trials.
Key Findings of the NIAGARA and HIMALAYA Trials
November 8th 2024In this episode of the Pharmaceutical Executive podcast, Shubh Goel, head of immuno-oncology, gastrointestinal tumors, US oncology business unit, AstraZeneca, discusses the findings of the NIAGARA trial in bladder cancer and the significance of the five-year overall survival data from the HIMALAYA trial, particularly the long-term efficacy of the STRIDE regimen for unresectable liver cancer.
Expanding Immune Response Testing to Support Vaccine Development
April 22nd 2025Nigel McCracken, chief operating officer, Virax Biolabs, discusses the expansion of its ViraxImmune platform into areas such as transplant monitoring, vaccine efficacy, latent virus reactivation, and CAR T cell therapy.
