The Adherence Fight: A TKO?
Why does the match against medicines compliance always seem to end in an easy knockout?
Healthcare professionals have been fighting an endless equivalent to the inspirational Rocky Balboa parable—with the exception that in this epic the ending remains unscripted.

Getty Images: spxChrome (Foreground gloves) / Aaron Cobbett (Background Frame)
A first glance at the current data screen actually suggests that patient adherence is getting worse, not better. New data from the Center for Health Transformation claims the annual cost of patients not taking their medicines as prescribed is nearly $300 billion, with approximately 125,000 patients dying each year due to poor adherence—that's 342 people every day. But the engagement of new stakeholders, tighter focus on wellness and prevention, and the development of better performance metrics to drive internal support for adherence programs could be adding the bulk the healthcare industry needs to finally make it a fair fight.
"I refer to this as the silent disease in America because of the large amount of non-adherence to medications, routinely in acute care situations but even more specifically in chronic disease," said Dr. Lyle Bootman, Dean and Professor at the University of Arizona School of Pharmacy in a recent adherence teleconference. "Not only is this a clinical problem in terms of [patient] outcomes ... it has serious economic consequences for this country. That $300 billion cost of non-adherence is in the same category and level of severity as heart disease and cancer, which are in the range of $250 billion to $350 billion to manage and diagnose. So, indeed, adherence, when looked upon as a disorder, is a very serious clinical and economic problem."
What is the true issue driving non-adherence? Shouldn't patients—especially those with chronic or more severe diseases—want to take their medication and feel better? Consensus is proving elusive; a variety of excuses exist. Patients start to feel better so they stop taking their scrips as often; they can't handle the unpleasant side effects; the copays are too expensive; or they just forget.
HealthPrize—an organization that provides pharmaceutical companies and other organizations with online adherence-incentive programs—scoffs at these factors as excuses that mask the true root of the problem. Its blunt and rather frightening conclusion is that medication non-adherence is often intentional. "Upon greater digging, it becomes clear that forgetfulness can also serve as a convenient excuse rather than a true reason," reads HealthPrize's recent white paper, "Medication Non-Adherence: An Ancient Problem in Need of Modern Solutions." "There are many deeper cultural reasons ... such as: taking medication is not a high enough priority; taking medication makes a person feel old; it reminds a person that they have a 'condition' or that they're a 'patient;' they don't trust their doctor; or they just don't like the idea of taking a pill."
If there's any doubt as to the validity of such a statement, consider the vast number (more than 20 percent according to a study from Harvard Medical School last year) of patients who receive a first-time scrip from their physician and then never even make it to the pharmacy to fill the initial prescription. These patients have made an active decision not to take a medication—despite a recent appointment and discussion with their doctor, whose advice they presumably willingly sought out to manage their condition.
A survey and white paper—"Patient Adherence: The Next Frontier in Patient Care"—from Paris-based Capgemini Consulting found that "on average, adherence levels drop over the course of the patient journey from 69 percent of patients filling their first prescription to 43 percent continuing their treatment as prescribed after six months." Additionally, the paper says, "It is also estimated that non-adherence results in an average per-drug loss of 36 percent in potential sales for a pharma company."
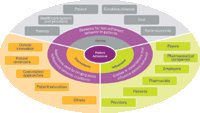
DIMENSIONS OF PATIENT ADHERENCE (Source: Capgemini Consulting)
Patient cost is also a theme, one that remains largely unspoken. A survey conducted in September 2010 by MDLinx and parent company M3 revealed that 95 percent of the nation's oncologists reported a rise in their patients' concerns over treatment costs in the six months prior to the survey. Of the 106 US oncologists surveyed, 84 percent said they had invested more time and effort into the financial planning of patients' treatments than they ever had before. Additionally, 67 percent of those who responded reported that their patients were rationing medications and/or forgoing treatment due to financial and insurance coverage concerns.
Setting Up the Match
Internal alignment within drug companies that strengthens the case for investing in adherence programs is another challenge; efforts that are disaggregated and fail to show a link between investment and outcome are victim to being seen as just another public relations exercise that makes the programs targets for budget cutters. "Patient adherence initiatives often lack a thorough understanding of the root causes of discontinuing treatment, or fail to engage patients sufficiently and to address the issue holistically," says the Capgemini white paper. "Individual tactics are tried by different brands and then discontinued as budgets and priorities shift, before their impact is known."
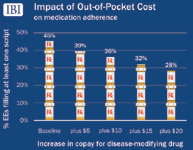
Source: Integrated Benefits Institute (EE = Employees)
Round 1: Building in Metrics
FICO's Health Care Practice division is now taking the same demographics tracking and analytics it has used since 1958 to come up with credit scores and applying those skills towards calculating non-adherence risk.

- Daria Blackwell, Founder, Knowledge Clinic
"FICO has, for the past 10 years or so, been providing data-based marketing solutions in the healthcare space," explains Todd Steffes, vice president of healthcare practice at FICO. Over the last few years, Steffes says, FICO's healthcare clients have been more focused on consumer marketing, and on how to better understand patients—including their reasons for non-adherence. "That's where this idea came from," says Steffes. "Could we apply our predictive modeling skill sets and the methodologies around how we do the credit scores toward the pharma space and help answer those kinds of business questions?"
The process of creating a Medication Adherence Score (MAS) began by partnering with pharmacy benefit manager MedImpact, which has access to claims data for patients across the country. Because the information from MedImpact is strictly demographic, it's all de-identified and HIPAA-compliant. FICO then used that data to determine which mixes of demographics were adhering to their medication in certain therapeutic areas. After a base study of 12 months, FICO can now use that data to predict the likelihood of adherence in other patient groups with similar mixes of demographics.
"What you're doing is looking at those initial patients—how they actually adhere and actually perform—and then analyzing their attributes and identifying which mix of those attributes is really predictive towards how they performed. That creates a scorecard that allows you to do the same analysis—using just publicly available data—for future patients," explains Steffes.
The upshot? FICO can then take this predictive data to pharmaceutical marketers, managed care organizations, and eventually physicians—all those who are at crucial points of contact with the patient—to help develop strategies to target the specific patient populations that are least likely to adhere.
Round 2: Knowledge Clinic
Another novel approach is leveraging the industry's educational mission for professionals to relate directly to the patient experience. With that goal in mind, Daria Blackwell—entrepreneur, 2011 Healthcare Businesswomen's Association (HBA) Star, and 2004 HBA president, recently founded Knowledge Clinic in Ireland.
Blackwell has been involved with medical marketing and medical communications for most of her career. But it was while working for Roche that Blackwell got the idea of creating some sort of continuing medical education (CME) for patients. "I started developing resources for physicians to help them understand how patients think, because patients coming from different backgrounds all think very differently about Western medicine and what physicians tell them," she explains. "So eventually we arrived at the thought that there really needs to be a separate discipline that helps patients accept the fact that they are responsible for their own health and that they have to partner with their healthcare professionals."
From there, Knowledge Clinic was born. Currently, Blackwell is in the middle of organizing what she calls a "pilot trial" of medical education via webinars and other learn-from-home options, "where people are recruited—as soon as they are diagnosed with a chronic disease—into an educational program where they will learn at their own pace and pass a couple of simple tests that will acknowledge what they've learned."
A big part of non-adherence is lack of patient education, says Blackwell. For example, she says, most people who are diagnosed with hypertension are asymptomatic. "And the doctor just tells them, 'Here, take this pill.' Most of the time the patient doesn't realize they're going to be on this for life. Most of the time they don't realize that if they discontinue it, there could be very serious problems. They don't realize that hypertension leads to problems down the line that could include stroke and heart disease."
Not only do patients not realize the consequences of non-adherence; they also don't place enough value on their medications. "AARP did a survey a few years ago that revealed more people were willing to spend money on cable television than on life-saving drugs," reiterates Blackwell.
The idea behind Knowledge Clinic, according to Blackwell, is that patients will learn how to manage their own health—including the value of medication adherence—in a way that is easy to understand, personalized, and is cognizant of cultural and religious differences. Additionally, rewards for completing educational workshops at Knowledge Clinic will help keep patients motivated. "Once they've passed a test, patients will get a certificate, which is redeemable for different rewards and products from different partners that will be participating with us who have a stake in the management of that particular health condition," Blackwell says. For example, patients with heart disease might redeem points for free classes at health centers or for workshops to reduce stress levels; asthmatics might redeem their points for products such as air purifiers and allergen-reducing mattress covers.
Adherence, says Blackwell, is not a responsibility that can rest solely on the shoulders of patients, or on the pharma manufacturers. "It's going to take everybody," she says. "People have been working on compliance and adherence for a long time, and nobody's quite figured all of it out. It makes sense that the more different factions cooperate towards improving adherence, the more successful we will be."
Round 3: HealthPrize Technologies
Like Knowledge Clinic, the people behind HealthPrize recognize the value of cooperation when it comes to putting on the gloves and going up against patient non-adherence. At first glance, the company's website seems a bit too ... fun ... to be taken seriously as a contender in the adherence fight. But such an approach might be just the motivation patients need. In a world of boring lectures about medications, overbearing reminders to talk to your health professional, and promotional DTC, HealthPrize's simple idea of offering money and rewards for adherence gets right to the point in a way patients can understand.
"Medication adherence can be viewed in the same light as other 'healthy behaviors' like exercise or healthy eating, where an 'on-again/off-again' pattern is common," says the HealthPrize white paper. "Most adults are educated enough to know that it's a good idea to exercise regularly. And most adults have access to free forms of exercise, like walking. Yet, how many adults still have trouble following through?"
The concept is simple: Patients find out about the HealthPrize website through their physician or pharmacy, and sign up to play educational games, earning points that are redeemable for physical objects, gift cards to top retailers, and the chance to enter sweepstakes for cash prizes. The idea here is that patients will respond to immediate, short-term satisfaction items such as gift cards, while at the same time learning more about their condition and the importance of taking their medicine as directed. "What we're trying to do is leverage concepts and lessons learned from consumer marketing and behavioral economics ... and make the process engaging and fun for the patients so that they remain on therapy for a longer duration of time," explains John Ruvane, VP of sales and business development for HealthPrize.
"There is fundamentally a value problem at the heart of the medication adherence crisis," says the white paper, echoing Blackwell's perspective on the subject. "In other words, patients don't take their medication enough because they don't value it enough. High value—or more accurately, high perceived value—is what makes a person remember to brush their teeth every morning (they don't want bad breath at work), or remember to catch their favorite television show every week at the right time (they enjoy it), or pay cash out of pocket for their dog to visit the veterinarian (unconditional love is treasured)."
To tie in with HealthPrize's goal of teaching patients to value their medication, the company recently announced a partnership with PSKW, a marketing company that focuses on brand loyalty and provides patient copay assistance programs for its pharmaceutical clients. "PSKW has great power in getting physicians to write scrips for branded medications that have a copay card associated with them," says Tom Kottler, CEO of HealthPrize.
"I believe the physician will intrinsically feel good about providing the prescription with a copay card because they know how important copay is to the patient, so they feel like they're providing something of value to the patient," explains Steve Freeman, chief operating officer of PSKW. Once PSKW provides the copay discount program and the physician prescribes the drug, the patient then opts in to use the discount card. Through the PSKW/HealhtPrize partnership, the next step at the point of contact (either the physician's office or the pharmacy) is for the doctor or pharmacist to make the patient aware of HealthPrize. In theory, PSKW's discounts will get the patient to fill the initial scrip, and driving them to HealthPrize from there will motivate them to stay adherent, filling subsequent scrips regularly.
Round 4: Center for Business Intelligence
The Center for Business Intelligence (CBI) has long recognized the merits of direct intervention geared to the patient. It holds an annual conference and awards ceremony each April devoted entirely to coming up with innovative ways to tackle the problem.
The focus at the 2011 conference was on shaping patient behavior, says Christen Smith, program manager at CBI. "The best way to do that is to find the key points of intervention with the patients and train those people who are having the most influence with the patient to institute more practices to improve adherence."
One of the biggest potential influences, according to the speakers at the conference, is pharmacists. A great deal of emphasis is being put on the pharmacist/patient interaction, she says, "to get the patient to explain more about why they aren't picking up their prescriptions on time, or not at all, or if they're taking them incorrectly."
Like Blackwell, Smith and others at CBI recognize the value of collaboration when it comes to facing an opponent such as non-adherence. "There was quite a bit of talk at the conference on those different partnerships," she says.
Going forward, Smith says, changes in the industry—including healthcare reform—will change the way pharma and other stakeholders approach adherence. "With providers being incentivized to improve outcomes and not just continually treat patients [through ACOs, for example], physicians and managed care are going to have a greater stake in adherence. They're not exactly penalized, but they may make less money or get less reimbursed if they don't improve patient outcomes. And one way to really improve those outcomes is through better adherence."
Round 5: National Consumer's League
Also making a new play to drive better patient adherence is the National Consumer's League (NCL). In May, NCL joined with US Surgeon General Dr. Regina M. Benjamin to launch a public education campaign to raise awareness among patients about the consequences of not taking medication as directed.
The campaign, "Script Your Future," features a website that offers "tools to support patient efforts to adhere to their prescribed medication, including text massage reminders, medication charts and lists to keep track of medications, and fact sheets on common chronic conditions," according to a NCL press release. The campaign is supported by a coalition of close to 100 public and private partners and sponsors, including healthcare professional groups, chronic disease groups, health insurance plans, pharmaceutical companies, consumer groups, and government agencies.
Script Your Future is focusing on three common chronic conditions: diabetes, cardiovascular (which includes high blood pressure and high cholesterol), and respiratory (which includes asthma and COPD).
"One way we're approaching this, based on the research that we've done, is that patients don't always understand their condition, and they don't always understand the consequences of not taking their medication," says Rebecca Burkholder, vice president of health policy for the NCL. "We conducted focus groups across the country with patients that had these chronic conditions. And what seemed to be effective for them was focusing on the consequences, on the impact that not taking your medication can have on not just you, but your family. If you don't take your medication as directed, you might not be around for your family—to enjoy moments together or to help take care of them."
Over the next three years, the campaign will provide materials through partnerships with pharmacies, hospitals, medical offices and clinics, and health insurance plans; host community events and health fairs; and evaluate medication adherence awareness through research.
Local radio spots, public service announcements (PSAs), and online videos are also part of the campaign, along with a sister website designed for physicians and other healthcare professionals, "because we know it's really important that they are very much involved, having that conversation with patients about their condition and their medicine—that's key," says Burkholder.
Overall, she says, the campaign "is about raising awareness as a step toward changing behavior." Later this year, Pharm Exec will participate in a Round Table discussion with the NCL to further discuss the problems and possible solutions surrounding adherence.
A New Champion?
Going forward, if pharma and other stakeholders are to win the fight against non-adherence, new strategies must be employed. One critical driver is focus—targeting the message to a degree that was missing in the past.
"Companies come up with these cross-product platforms that address the issues related to adherence, and they expect them to work in diabetes, cancer, overactive bladder, multiple sclerosis, and all these other conditions," notes Vernon Schabert, senior principal in the Health and Economics Outcomes Research practice at IMS Consulting group, "when really, every single one of these therapeutic areas has different populations with different concerns, different symptoms, different cost burdens, and so on. And so it's really important when you're looking at adherence as a solution to say, 'What does it mean for this specific product and this specific therapy area?'"
With these cited new initiatives from NCL, Knowledge Clinic, and other concerned organizations and stakeholders around the world, it may just be possible for industry to score a momentum-shifting blow in the adherence fight. As the Capgemini white paper puts it: "Understanding of the issue has evolved from the narrow scope of compliance, which places the entire responsibility on a passive patient, to a broader definition where adherence is a more collective responsibility between healthcare providers and patients who are active participants in their own care."

The Misinformation Maze: Navigating Public Health in the Digital Age
March 11th 2025Jennifer Butler, chief commercial officer of Pleio, discusses misinformation's threat to public health, where patients are turning for trustworthy health information, the industry's pivot to peer-to-patient strategies to educate patients, and more.
Navigating Distrust: Pharma in the Age of Social Media
February 18th 2025Ian Baer, Founder and CEO of Sooth, discusses how the growing distrust in social media will impact industry marketing strategies and the relationships between pharmaceutical companies and the patients they aim to serve. He also explains dark social, how to combat misinformation, closing the trust gap, and more.